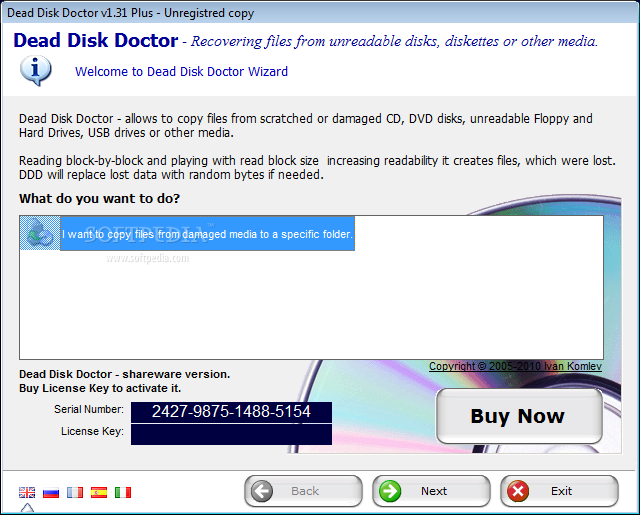
By this technique, the surgeon can get as close as possible to the level of the internal cervical os by the vaginal route. A stitch (usually silk or other non‐absorbable material) is inserted around the cervix, enclosing it. The anterior vaginal wall is cut under anaesthesia and the bladder is reflected (pushed) back and upwards. 
Shirodkar 1955 reported the insertion of a cervical stitch (suture) at around 14 weeks of pregnancy. All interventions require at least regional anaesthesia in the form of a spinal or epidural block. There are a number of proposed treatments designed to keep the cervix closed until the expected time of birth. Cervical incompetence has traditionally been viewed as an 'all or nothing' condition, but the concept of it being a continuum, responsible for some pre‐term deliveries as well as mid‐trimester miscarriages is now gaining in acceptance. In the absence of previous surgical trauma (cervical surgery), the underlying pathogenesis of cervical incompetence is often unknown. 
The diagnosis is more often based on history of recurrent mid trimester losses ( Stirrat 1999) or previous mechanical (physical) dilatation of the cervix during surgery. A shortened cervical length may increase the likelihood of preterm labour ( Murakawa 1993). Pre‐pregnancy diagnostic tests may include hysterosalpingogram (an investigation where dye is passed through the cervix and uterus and x‐ray pictures taken) or more recently transvaginal ultrasonography measuring cervical length. In developed/resource rich countries an unborn baby is considered to be viable at 24 weeks and in resource poor/developing countries viability is still 28 weeks. Gestational age distinguishes between a miscarriage (0 to 23 weeks 6 days) and pre‐term labour (24 to 37 completed weeks). Other definitions of cervical incompetence used include: 'recurrent second trimester or early third trimester loss of pregnancy caused by the inability of the uterine cervix to retain a pregnancy until term' ( Althuisius 2001a) and 'a physical defect in the strength of the cervical tissue that is either congenital (inherited) or acquired' (caused by previous damage) Rust 2000a. Passage of a 9mm Hegar dilator through the cervix without resistance, in a non‐pregnant women is indicative but not diagnostic of cervical incompetence. Some workers have defined cervical incompetence as 'the history of painless dilatation of the cervix resulting in second or early third trimester delivery and the passage without resistance, of size nine Hegar dilator (an instrument which is used to measure the size of cervical dilatation in millimetres i.e. 
There is, however, no consistent definition of cervical incompetence ( Berry 1995) which hampers knowledge of the true incidence. This may be due to cervical weakness (incompetence) if the miscarriage occurs in the second (12 to 23 weeks 6 days) or early third trimester (after 24 weeks).Ĭervical incompetence during pregnancy has been described as early as the seventeenth century ( Riverius 1658) and complicates about one per cent of an obstetric population ( McDonald 1980) and eight per cent of a recurrent miscarriage population who have suffered mid trimester pregnancy losses ( Drakeley 1998). For a few women, this process seems to recur in subsequent pregnancies. Occasionally the cervix starts to open early in the pregnancy, leading to a miscarriage. At the onset of labour, the cervix begins to dilate, ready for the baby to be born. The cervix normally stays tightly closed during pregnancy, with a mucus plug sealing the opening. Extreme prematurity can also have severe implications as babies that survive may have residual handicap. Pregnancy loss at any stage is distressing but especially so when this happens later on in the pregnancy.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
